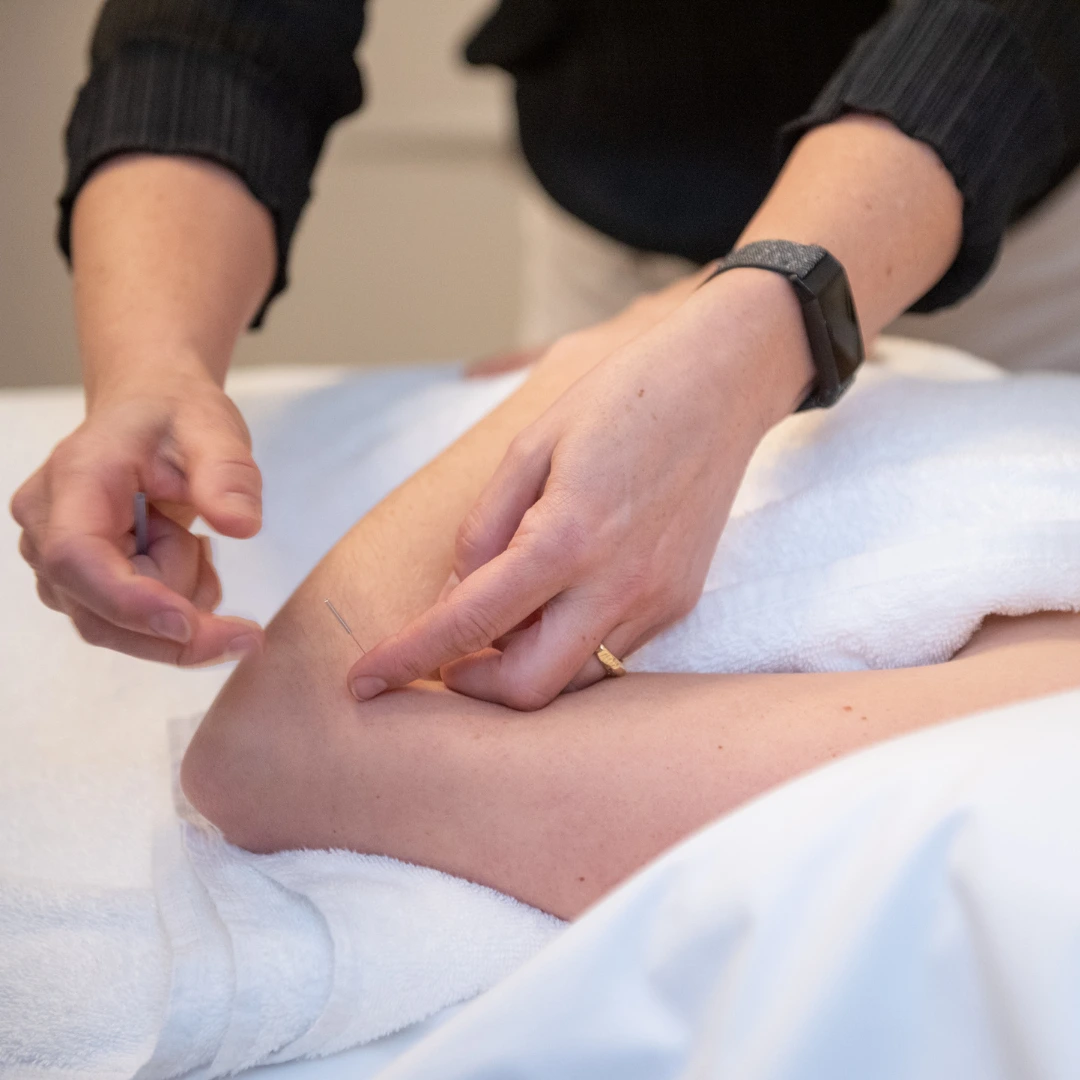
Are you passionate about supporting people on their fertility, pregnancy, or new parenthood journey? Do you love working with those trying to conceive, undergoing IVF, or navigating pregnancy and postpartum recovery?
We’re looking for a skilled and caring massage therapist to join our team at Fertile Ground Health Group – one of Melbourne’s most highly regarded fertility and perinatal practices in natural health. This is a unique opportunity to grow your massage career in a purpose-driven, collaborative, and supportive environment.
Why Choose Fertile Ground Health Group?
For over 25 years, Fertile Ground has been synonymous with exceptional care in reproductive medicine. Our practitioners are well respected among medical specialists and industry experts. We pride ourselves in providing care defined by integrity, compassion, and expertise.
Collaboration and co-creation are at the heart of how we work. We believe this shared approach creates the richest learning environment – one where practitioners, patients, and the entire support team benefit. It’s a space that fosters continuous growth, connection, and professional evolution.
Massage Therapist Position Eligibility
To be eligible for this position, you already have passion, interest and experience as a Massage Therapist in fertility, pregnancy and/or postpartum massage, and beyond. Ideally, you love working with people trying to conceive, those who are pregnant and new parents, and you want to simplify your practice to focus on being a fantastic practitioner and dedicating your efforts to growing your patient reach and massage career with the support of Fertile Ground.
Great skills and passion for massage is required, along with your desire to develop referrer relationships (with our help) to achieve collaborative patient results. Additional training in fertility or pregnancy massage will be highly regarded, but not essential. Mentoring is available for our signature treatments for fertility, pregnancy, and postpartum (mother roasting) massage.
What We Offer
You’ll receive dedicated business management and admin support, so you can focus on what you do best – caring for your patients. You’ll be part of a collaborative team of well-known and respected professionals, with opportunities to co-create, grow, and thrive in your career.
At Fertile Ground, we support you from every angle – with the tools, mentoring, and guidance to develop your professional profile and build a fulfilling practice. With new patients ready and waiting, and the strength of our trusted reputation behind you, you’ll have the opportunity to grow a thriving, full practice with ease.
What We’re Looking For
We are looking for an experienced Massage Therapist who:
- Is ready to hit the ground to establish a fulfilling practice.
- Values collaboration and has an ability to develop referrer relationships and patient results.
- Is willing and wants to establish themselves as a leader in the massage profession.
- Understands the value of community cultivation, through methods such as social media, writing blogs, potential speaking opportunities (to health professionals or patient groups), and/or running small workshops, classes or support groups (in person or online).
Massage Session Times
You will need to commit to a minimum of two massage sessions (days) per week, with a minimum of 4 massages per session. There is immediate room for more sessions than this or growth if desired. You will be working in one of Australia’s most intentionally beautiful and vibrant clinic spaces with an extensive dispensary supplying the entire clinic’s prescription needs at The Melbourne Apothecary.
Room availability:
- Monday
- Tuesday
- Wednesday
- Friday
- Saturday
Apply Today
If you’re ready to take the next step in your career, email your cover letter and resume to Sarah Sanelli, Practice Manager, at management@fertileground.com.au.
“Touch was never meant to be a luxury, it’s a basic human need.” – Irene Smith